MEDITECH Surveillance Rules Engine
Overview
In MEDITECH 6.1, the Surveillance dictionaries are housed under Quality Management. Both Quality and Clinical staff will use these tools to monitor the patient population.

Surveillance Fact Dictionary
The Surveillance Rules engine functions differently than the Rules Engine used to apply clinical decision support in ordering and documentation. These rules are comprised of “Facts”. Each fact is built out separately and then added to the rule it’s going to be applied to.
The design philosophy behind this was to avoid “reinventing the wheel”. For instance, a “Fact” could say, only look at the INPATIENT population or only assess if a problem wasn’t present on admission. Once facts are built they can be applied to many different rules that assess for different things.
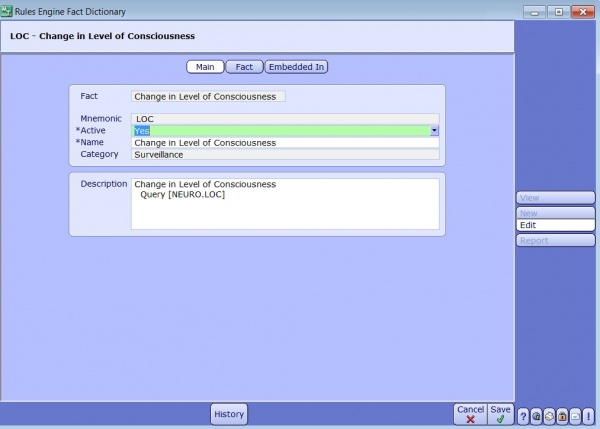
The above fact will assess the patient for a change in the level of consciousness. This fact will most likely be used is assessing the patient population for a variety of conditions: UTI, Dementia, Stroke, VAP and Sepsis for example all use these criteria.
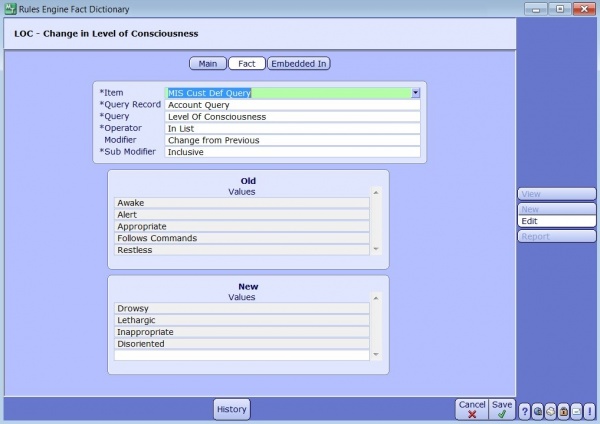
Depending on the Item, (field, query, lab value etc) operator and modifier you are assessing you will be presented with different options to further define your “fact”. If your modifier is just “Equals” than you will not have to define old and new values.
In the example above, we are looking for a delta change. If the patient was one of the old values: Alert, Awake, Follows Commands and that changes to Drowsy, Lethargic, or Disoriented then we want to trigger a flag. This fact could be used on its own OR in combination with other facts. Perhaps we only want to trigger a flag if the patients level of consciousness changes AND they have increasingly low urine output.
Fun Fact: Greek Letters are not just for frats! They can be found in mathematics, finance, science and engineering. The Delta symbol represents a finite change (math), a sensitivity to price (finance), heat (chemistry) and the degree of freedom in two pooled populations (statistics). It’s all Greek to me though!
Surveillance Rules Dictionary
Once we have built our facts we can attach them to a Rule. In the next example we can see how multiple facts can be combined to make a rule.
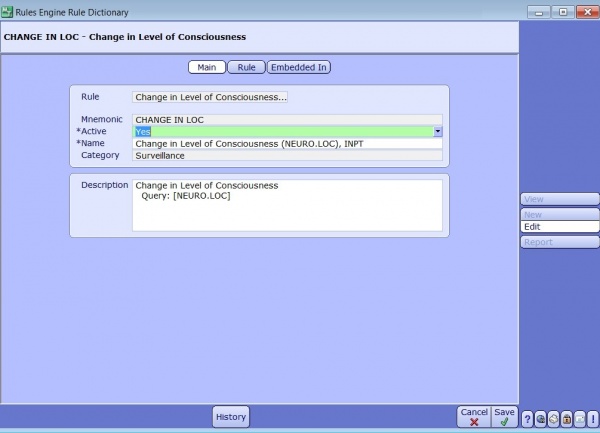
On the main tab you can define what your rule will assess. Use the description tab to clarify the goal you want to achieve and list any queries that might be mapped in the rule.
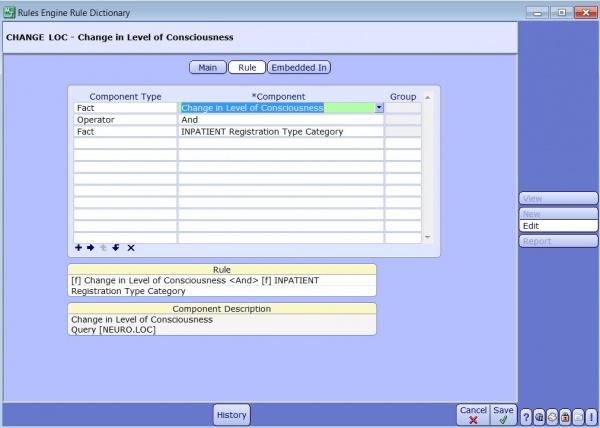
The Rule tab is where you pull in all your facts, use the operator between facts to give your rule direction. In the example above we want to assess only the inpatient population for a change in consciousness. The operator AND combines the two, whereas OR would look for either fact to trigger the rule. Placing facts into groups helps organize your rule logic by adding a unique order to the assessment.
Once your Rule has been created make sure to rebuild the surveillance rules. This only needs to be done once initially and then subsequently with additional edits. In the Rules Engine Build Dictionary, build your rule by building (or rebuilding) the Surveillance Category.
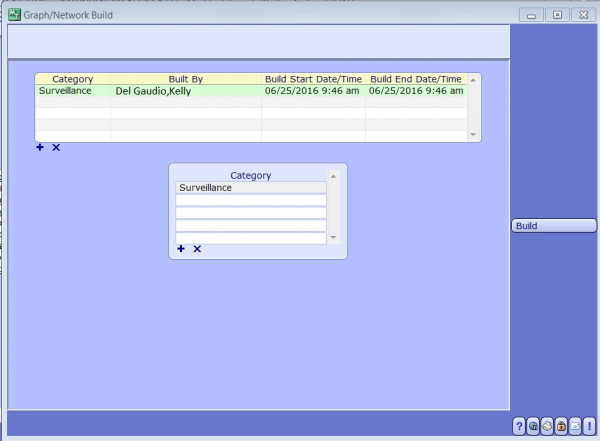
Surveillance Rules Engine Validation
Once the build is complete, it can be tested on a patient to verify it works correctly. Add the criteria to a test patient and then use the rule verification tool to make sure that patient is properly flagged. In the next example, make sure your test patient has a lactic acid level greater than 2. This helps you verify that you’ve got your facts straight (pun intended).

Surveillance Profile
After building the rules, they can now be associated to a Surveillance Profile. These profiles can have 2 types of rules associated to them. Qualifying (The patient has met the criteria and has been added to the watchboard) or Removal (The patient no longer is at risk)
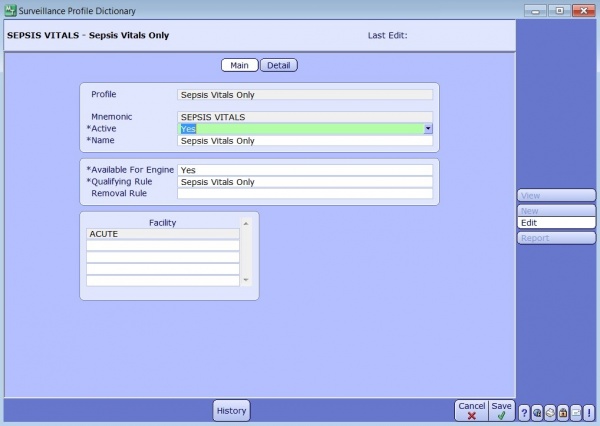
Galen Pro Tip: Make the rule “Available for Engine” if you want this profile to actively assess the population for patients at risk.
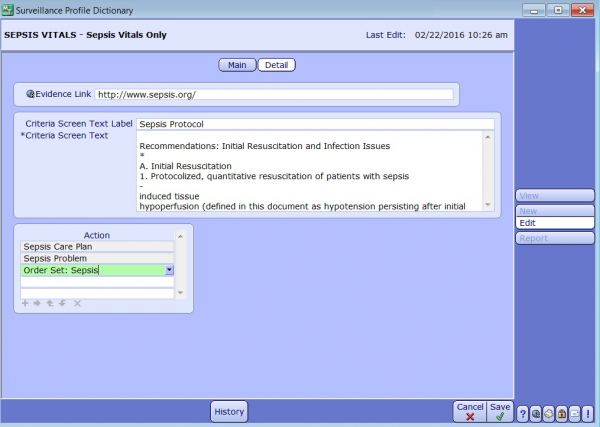
The Detail section of the Surveillance Profile is where you can define the criteria used to assess the patients and add an evidence link that can be accessed by the clinical and quality staff for further research on the topic. This is also where actions can be defined. It is important to build appropriate actions based on the patient event.
Stay Tuned: In a future blog, I will discuss Conditional and Protocol based order sets that drive care based on the patients current and preexisting conditions and are compliant with hospital protocols, standards and guidelines.
Surveillance Action
Actions are defined in the Action Dictionary and can be restricted to facility or role.
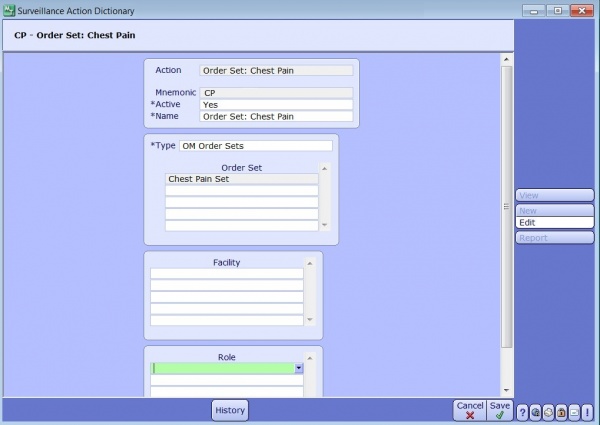
The following types of actions can be created at aide staff in initiating treatment plans and therapies for flagged patients:
- Add a document template
- Add a PCM Problem
- Send a message
- Generate an Order
- Generate an Order Set
- Add a Pathway or Care Plan
- Add Intervention
- Add Intervention Set
- Add a PCS problem
Surveillance Roles
Surveillance Roles are created in the Surveillance Role Dictionary to restrict allowable actions to a type of user. They also indicate if the user has access to manually add or remove patients from the Watchlist.
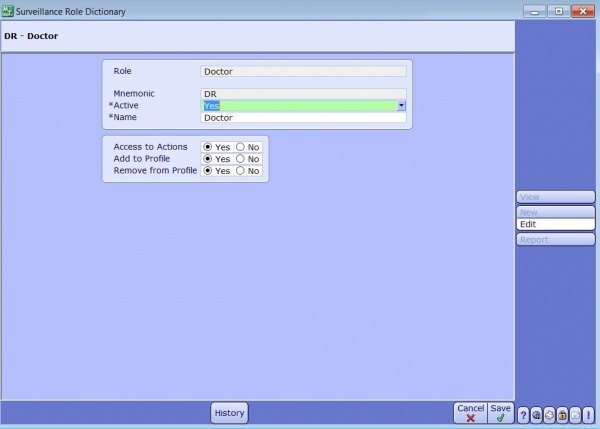
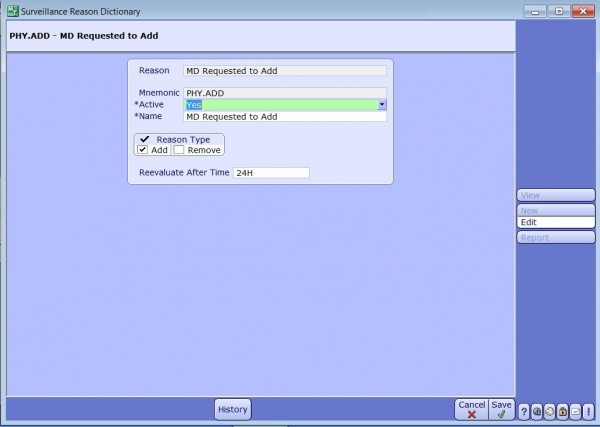
If your assigned role indicates you have access to add or remove patients from boards you must indicate a reason when doing so. These reasons are defined in the Surveillance Reason Dictionary and can be used to track contraindications for patients that have been flagged or monitor patients that don’t meet all criteria.
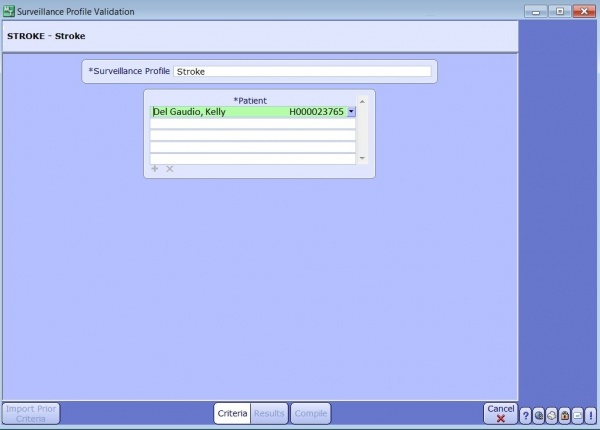
Surveillance Profile Validation
Once a Surveillance Profile has been built you can use the Surveillance Profile Validation tool to check your rules on a patient. This makes sure your setup is correct.
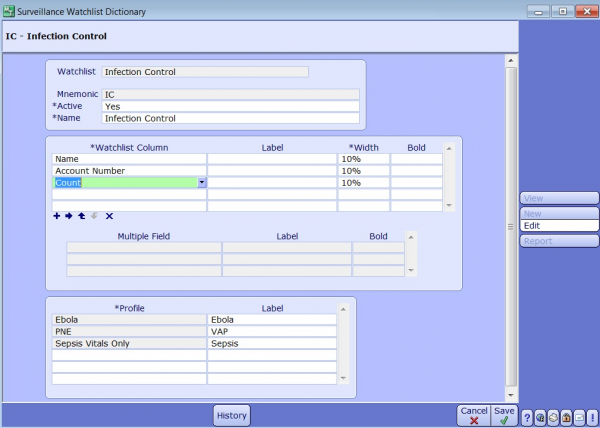
Surveillance Watchlist Dictionary
The Surveillance Watchlist Dictionary is where multiple profiles can be assigned to a user group, for instance: Infection Control or Quality Nurses. Add the columns you want on your Watchlist (most likely patient identifiers) and then the individual profiles in the profile section below.
When assigned a Watchlist, Infection Control and Quality staff will be able to see all profiles assigned to them simultaneously. They can open the patients chart or select the “Go To” option to view the condition specific board.

Challenge: Can you name the actor that’s played all the patients on the Quality Surveillance Board?
Hint: They’re all wild and crazy guys!
Surveillance - Quality Access Dictionary
The Surveillance Tab in the Quality Access Dictionary helps to define and customize your default watchlist’s by user group, the frequency in which they refresh and the qualifying and non-qualifying indicator icons that display.
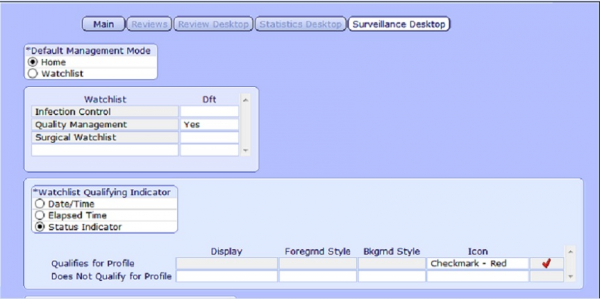
The last step is creating conditional display boards that display pertinent information about the patients worsening condition. Below is a VTE display board that will pull information from all areas of the patients chart and display them in a meaningful way to a clinician assessing for VTE.
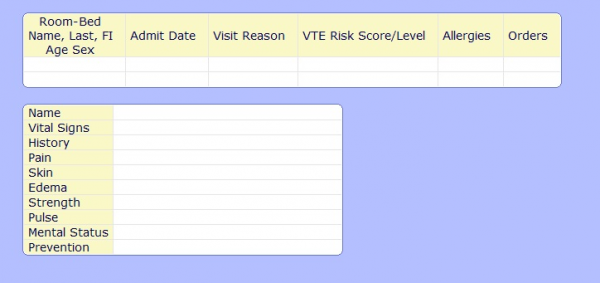
Quality and Infection control staff aren’t the only ones who will benefit from these display boards. Nurses can have access to them too by adding the Surveillance Type ID method in the PCS/EDM Access Dictionary. The Nurse can then toggle between boards using the lists option from their menu.
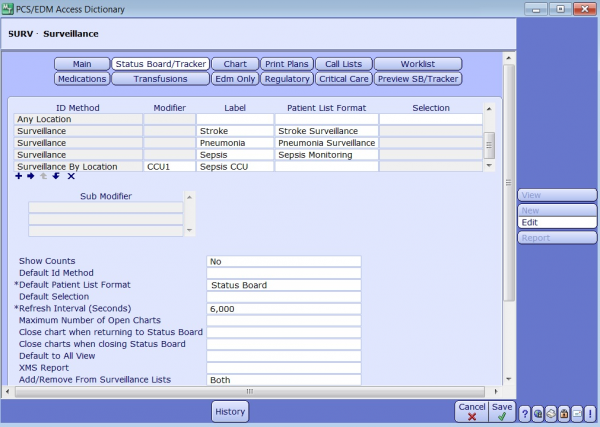
Access settings above also dictate if the nurse will have access to add or remove patients from a surveillance list. Also note that display boards can be built and utilized even if you are not on MEDITECH 6.1 and do not have the predictive rules engine.
See Appendix A below to see an example of how the concepts and setup in this guide can be applied to VAP monitoring.
Appendix A
Applying what we’ve learned.
If we were assessing a patient at risk for Ventilator Associated Pneumonia, what type of information would we need to see and what kind of facts can be built to trigger a flag? The board display criteria works in combination with the facts in the rule, so its best practice to build these together. Here are some common examples to get you started:
Fact: [f] is the patient intubated >48 hours (my recommendation is 36 hours which gives you time to be proactive)
Board Criteria:
| Patient Intubated/On Vent | Type | Duration |
Fact: [f] ordered/administered antimicrobial agents
Board Criteria:
| Orders | Antimicrobial Agents |
Rule comprised of facts: [f] chest radiographic examination order AND [f] change in one or more of the following: infiltrate OR consolidation OR cavitation’s OR pleural effusion AND [f] one or more of the following: new onset of purulent sputum OR change in character of sputum AND/OR [f] organisms cultured from blood AND/OR [f] isolation of an etiologic agent from a specimen obtained by transtracheal aspirate OR [f] bronchial brushing or biopsy AND/OR [f] increased or decreased white blood cell count AND/OR [f] increased temperature.
Board Criteria:
| Lab Results | Vital Signs | Chest X-ray (image and interpretation) |
Facts: [f] daily minimum PEEP increase OR [f] increase in the daily minimum FiO2 of ≥ 0.20 (20%)
Board Criteria:
| Daily Minimum PEEP | Daily Minimum Fi02 |
Other Board Criteria should include:
| Board Criteria |
| Identifying Demographics (Because duh) |
| DVT risk or prophylaxis |
| PUD risk or prophylaxis |
| Worsening Oxygenation/Onset of worsening oxygenation |
| Bed Elevation (should be at 35-45 degrees) |
| LRT orders/results |
| Lab Ratio Indicators |
| Evidence of Blood Stream Infection |
Taking Action
Actionable Order Sets can also be created, using rules to assess the patient for preexisting conditions and other factors to ensure optimal success of the therapy chosen. Death or complications are statistically lower in patients that receive the appropriate initial antibiotic treatment compared with patients requiring a treatment change. Which is why getting it right the first time is crucial.
If the patient has no known risk factors for multi-drug resistant pathogens and the suspected VAP is early onset we may place them on a Limited Spectrum Antibiotic Therapy but if they have recently been administered antibiotics or they have risk factors for MDR organisms, then we would initiate a broad spectrum antibiotic therapy. Web links to evidence based medicine sites can also be added to further assist with the decision process.
Our goal at Galen Healthcare Solutions is to help your hospital build Surveillance tools that will have your clinicians working smarter, not harder; giving them more time to do what they do best: Patient Care.